Measuring Patient Experience
Most Australian dentists are now aware of the imperative to enhance patient experience. Not only does a patient-focused practice lead to altruistic fulfillment, it also makes financial sense. The cost of investing in a new patient or client is recognised in conventional business wisdom as costing up to ten times more than retaining an existing customer.
Thus, it stands to reason that more practice owners are taking measures to uncover retention solutions that will encourage loyalty, ‘raving fans’ (positive online reviews) and referrals. Assessing the issues that influence patient engagement, such as patient partnerships, reducing wait times, reducing pain, and providing effective and reliable care, is a key place to start.
Metrics and data capturing of patient experiences are constantly growing more sophisticated, leading to a wealth of information that allows for deep insights into the patient experience. There has been a trend of increased access to an abundance of government and peak body reports, online reviews and even language processors that seek deeper understandings of the qualitative data generated by patient comments.
Although these methods are invaluable in understanding the big picture, they rely on large datasets. By consolidating answers and generalising data, large-scale analysis can lead to dangerous assumptions that miss the all important ‘why’ and fail to take case-by-case causes into account. It is vital to look beyond percentiles and trends when attempting to understand how your unique dental practice can look at patient satisfaction to reach retention goals.
As a supplement to large datasets, there are ways to measure patient experience that rely on qualitative observations. This approach is an opportunity to gain deeper insights into what your most valuable asset, existing patients, are experiencing in your practice and will allow you to make informed conclusions to subsequently improve that experience.
Introducing: Design Thinking
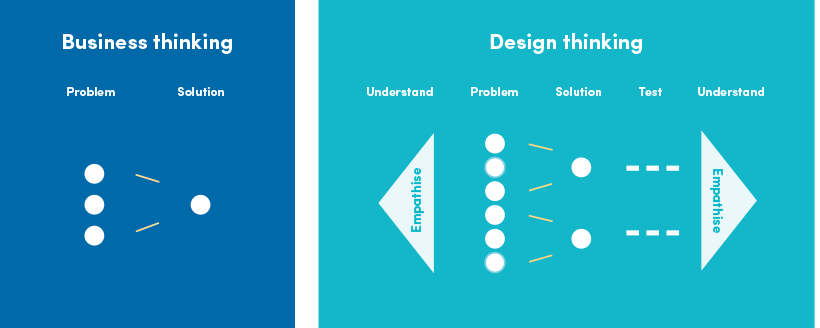
Sharon H. Kim, Christopher G. Myers and Lisa Allen’s recent piece for Harvard Business Review argues that one of the most promising developments in qualitative patient experience studies is the application of design thinking–a creative, human-centered problem-solving approach that leverages empathy, collective idea generation, and continuous testing to tackle complex challenges. Unlike traditional approaches to problem solving, design thinking focuses on understanding patients and their experiences, before coming up with solutions. Design thinking can allow you to uncover relevant information, better understand cause and effect, and test solutions before assessing resulting experiences.
There are no black-and-white templates on how to implement design thinking. However, working within the concept’s loose confines by engaging with patients closely and using processes such as empathy mapping is an excellent way to start enhancing your practice’s patient experience.
The concept of empathy mapping originated in design thinking. Empathy mapping is based on identifying people’s various emotions as they navigate through an experience. An empathy map grades the intensity of emotions during one experience, ranging from fear, anxiety, surprise, delight, confusion, anger, reassurance, comfort, and peace of mind. It can be offered to patients to fill out themselves, or used as a reference point when observing patients. To try out an empathy map, you can download a template by clicking here.
The Waiting Room Test
Research suggests that the waiting room experience is a significant contributor to overall patient satisfaction. Large scale data demonstrates that reducing waiting times to less than 10 minutes increases patient satisfaction.
It’s not always possible to commit to less waiting time, as much as we would love to. This is where design thinking comes in. A design thinking approach would aim to explore a creative solution by uncovering new ways of helping patients feel comfortable enough that they enjoy, and even recommend, their experience. A window into the patient’s emotions should be a strong motivator in assessing a redesign of care experiences.
By observing your patient’s’ body language, facial expressions and responses, as well as asking how the patient is feeling, you gain enough insight to begin to understand the experience from their perspective. With this understanding, you can introduce potential solutions, while continuing to monitor the patient’s responses.
.
If patients are observed as (example):
- Bored – consider introducing free Wi-Fi or magazine rack
- Frustrated – consider introducing text alerts with waiting time estimates, or ensure that staff members clearly communicating waiting times to better manage expectations
- Uncomfortable – consider the look of the room. Could evidence-based ‘anti-anxiety’ art assist? How can you design and decorate your waiting room in a way that appeals to the emotions?
The designing thinking process should guide you, the facilitator, to empathise with patients, think creatively, prototype, and continually test solutions to these problems.
Improving the patient experience should be every Australian healthcare provider’s mission. Design thinking is an accessible and insightful process for achieving this.



